“It’s Amazing What You Can Achieve One Day at a Time”
In December 2014, Kirsty’s life changed in an instant.
Pregnant with her second child and working as an exam supervisor, she experienced a severe headache that lasted for days. At the time, it didn’t seem like anything serious. A doctor suggested dehydration. She drank more water. The pain disappeared.
Life moved on.
Until the day her daughter was due.
A Seizure No One Expected
On the morning of her planned home birth, Kirsty had a tonic-clonic seizure.
“It really scared my husband,” she recalls.
She was rushed to the hospital, where doctors initially suspected preeclampsia. Her daughter was delivered that same day safely, but the seizures didn’t stop.
By that evening, it was clear something else was wrong.
Kirsty doesn’t remember much of what happened next.
“I woke up two days later and thought I was dead.”
Soon after, a surgeon delivered the words that would redefine everything:
“You have brain cancer.”
Watch Kirsty tell her story in full in the Aunty M Brain Tumours Talk Show interview below, or keep reading for the written version
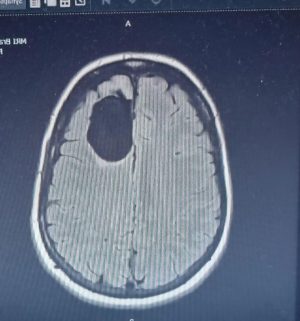
Diagnosis: Diffuse Astrocytoma
Kirsty was diagnosed with a grade two diffuse astrocytoma, a slow-growing but incurable brain tumour.
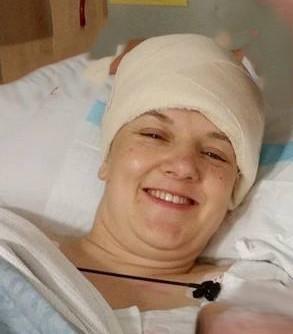
Her first surgery took place just weeks later, in January 2015.
Although surgeons removed as much of the tumour as possible, diffuse astrocytomas are infiltrative — meaning microscopic cells remain.
“She told me it would come back,”
 |
 |
Living Scan to Scan
The years that followed were defined by “watch and wait” — regular scans every few months.
With that came a familiar experience for many patients:
Scanxiety.
“You build up to the scan, then you wait for results… and then you decompress. It’s a cycle.”
At times, Kirsty says she only had a few weeks of relief between waves of anxiety.
To cope, she created an inner strategy:
“I imagined a little version of me called Scarlet. I would tell her, ‘You’re safe. We’ll get through this.’”
Motherhood in the Middle of Trauma
Kirsty was navigating far more than a diagnosis.
She had a newborn baby, a four-year-old child, and — at the time — very little family support nearby.
Complications from her seizure left her with three spinal fractures and ongoing weakness on her right side.
Even breastfeeding became too painful.
Despite everything, her children became a source of strength.
“They’ve grown up with this being normal,” she says. “They understand when I need to rest or when things are too loud.”
Surgery, Setbacks, and Starting Again
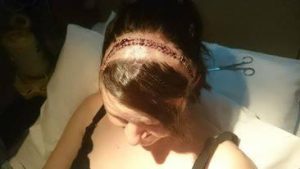
Six years later, Kirsty underwent a second brain surgery.
This time was harder.
She was now living through a divorce, had limited support, and afterwards experienced depression — partly due to the tumour’s location in the left frontal lobe, which affects emotional regulation.
“It’s a grief process,” she explains.
“You lose the life you had and have to learn your ‘new normal.’”
But she also found strength in unexpected places — particularly her community.
“People brought food, helped with the kids, drove me to appointments. I felt incredibly supported.”
A Turning Point: New Treatment Options
In 2021, Kirsty was told she would likely need radiotherapy and chemotherapy.
Then something changed.
Her oncologist introduced her to a gene-targeting therapy trial — a newer, more personalised approach to treatment.
“It felt like a gateway opened,” she says. “Like — here’s your life back.”
That moment sparked a shift.
Instead of living six months at a time, Kirsty began planning again.
Rebuilding Purpose
Before her diagnosis, Kirsty had completed an undergraduate degree in psychology.
After treatment, she returned to that passion — but in a new way.
She trained as a crisis counsellor with Lifeline Australia.
“It gave me my purpose back,” she says.
Managing fatigue remains a daily challenge — something she’s had to learn to accept.
“I used to do five things at once. Now I listen to my body.”
She has also returned to university part-time, adapting to a new way of learning with support from disability services.
 |
 |
“TuMerd”: Turning Pain Into Connection
In the early days of her diagnosis, Kirsty noticed something missing:
There was very little hopeful, human conversation about brain cancer online.
So she created her own space.
TuMerd — a play on words (and a very honest reflection of how she felt about her tumour).
Through social media, she began sharing her journey, raising awareness, and connecting with others around the world.
“I went from feeling alone to building a global village.”
Today, her platform continues to offer support, humour, and honesty to others navigating similar paths.
Strength, Recovery, and Redefining Life
Kirsty still lives with the physical effects of her tumour and surgeries — including balance issues and sensory sensitivity.
She uses strength training (including CrossFit-style workouts) as part of her rehabilitation.
“It’s taken 11 years, but I’ve built my strength back.”
Now, more than a decade after her diagnosis, she says:
“I feel the best I’ve ever felt.”
One Day at a Time
Kirsty’s story isn’t about a neat ending or a cure.
It’s about resilience, adaptation, and choosing to keep going — even with uncertainty.
Her message is simple, but powerful:
“It’s amazing what you can achieve, one day at a time.”
Understanding Diffuse Astrocytoma & Pregnancy
What is a Diffuse Astrocytoma?
A diffuse astrocytoma is a type of brain tumour that develops from star-shaped cells in the brain called astrocytes.
- It is considered a low-grade (grade 2) glioma
- It grows slowly, but spreads into the surrounding brain tissue
- This means it can’t be fully removed, even with surgery
- Over time, it can regrow or transform into a higher-grade tumour
Even when scans look “clear,” microscopic tumour cells often remain, which is why ongoing monitoring is essential
Why Kirsty Needed Ongoing Scans (“Watch and Wait”)
Diffuse astrocytomas are often managed with a strategy called:
“Watch and wait”
This involves:
- Regular MRI scans
- Monitoring for changes or regrowth
- Delaying treatments like radiotherapy for as long as possible
This approach helps preserve quality of life while the tumour remains stable.
Brain Tumours During Pregnancy: What Happens?
Kirsty’s story highlights something many people don’t realise:
👉 It is possible to have a brain tumour during pregnancy and still have a healthy baby
Brain tumours in pregnancy are rare, but they do happen
Key medical considerations include:
- Hormonal changes and increased blood volume during pregnancy can sometimes affect tumour behaviour or symptoms
- Some women may experience new or worsening symptoms, such as seizures
- Each case is managed individually by a multidisciplinary team (neurology, oncology, obstetrics)
Can Babies Be Born Healthy?
Yes — and Kirsty’s story is a powerful example of this.
Research and case studies show that:
- Many women with gliomas (including astrocytomas) can have successful pregnancies and healthy babies
- Pregnancy does not appear to reduce overall survival in low-grade glioma patients
- With careful monitoring, both mother and baby can be safely supported
In some cases, treatment may be:
- Delayed until after delivery
- Adjusted to reduce risk to the baby
- Carefully timed around the pregnancy
Why Seizures Can Be a First Symptom
For many people (like Kirsty), a seizure is the first sign of a brain tumour.
This happens because:
- The tumour disrupts normal brain signals
- Pressure or irritation in the brain can trigger abnormal electrical activity
Seizures during pregnancy are always taken seriously, as they can affect both mother and baby, which is why urgent medical care is essential.
The Takeaway
Kirsty’s experience reflects both the medical complexity and the hope within a brain tumour diagnosis:
- Diffuse astrocytomas are serious but often slow-growing
- Pregnancy with a brain tumour is rare, but possible to manage safely
- Many women go on to have healthy children and meaningful lives
Find Kirsty on Instagram and Facebook
View this post on Instagram