Claire Sutton from Southport, a registered nurse and a ‘Digital Transformation Lead,’ was living the life she always wanted. That was up until May 2020. It was the middle of the Coronavirus Pandemic, and the United Kingdom was in lockdown. Absolutely nobody wanted to be anywhere near a hospital.
Sadly Claire had no choice, she was struck by a paralyzing headache, and as a Registered Nurse she knew there was something very wrong with her, it was not like any normal headache she had felt. An ambulance was called, and she was in the A&E department having scan after scan, surrounded by doctors and nurses with facemasks on.
To make it even worse, Claire’s father sadly died of brain cancer in 2007. How do you not worry that you are about to go through the same journey as he did? It can feel so unfair to be tested so cruelly, and yet you have to do it all alone as you are not allowed any family or friends with you.
Here is Claire’s Brain Tumour Story:
Claire: My father passed away in 2007 from a Glioblastoma Multiforme. He was courageous throughout his diagnosis and his treatments and never moaned once. Sadly there was no treatment to save him and he passed away a year after his diagnosis. I was very aware of brain tumours but never thought I would get one myself.
I’ve always had migraines since I was about 10. Still, since being around 20 when I started with hormonal contraception, these have been infrequent. They went from twice a month to every month, to maybe one or two a year.
It was on the 10th May 2020. I was chatting with my mum when I felt a sudden excruciating pain in my head. It was the worst headache I had ever had. I went up to my bed to lie down and managed to text message one word to her: “help”.
I knew straight away this wasn’t a migraine, as my migraines always follow the same pattern of nausea, and a purple watery aura and take at least 30 minutes to develop which gives me time to take a naratriptan pill and go to bed – these work so well that I literally cannot remember the last time I had a migraine that got as far as the pain stage. I genuinely thought I was dying.
Ambulance Needed
My mum immediately called for an ambulance, they kept asking her if I’d been out the night before or if I had any Covid-19 symptoms. Soon an ambulance turned up and took me to hospital. The A&E department was initially concerned that I had a subarachnoid haemorrhage which is a brain bleed/stroke.
They said I would be in the hospital for a few days with tests, no family or friends could come and see me which meant that not only did I have to go through this alone, I also had no clothes or overnight bag. Thankfully, my best friend’s mother in law is a paramedic and snuck in for a visit and brought some stuff.
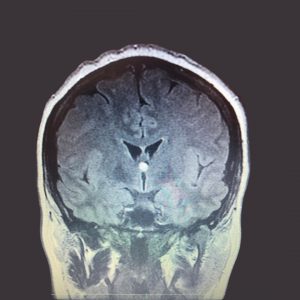
It was then that they found what they initially described as an incidental finding of a colloid cyst! I was in the hospital for five days having tests and was referred to neurology for a follow-up. At that point, I could go home, and they would be in touch about any treatment needed.
Misread Diagnosis
About a week after I was discharged, I re-read my discharge letter and panicked myself! I really thought it said I had an arachnoid cyst when I was in the hospital, which is a much less terrifying prospect than a colloid cyst. I thought I was just going to be on Watch and Wait.
When I realised it was a colloid cyst I called my GP and asked if they could refer me to neurosurgery instead of neurology which they did. My GP is amazing – having also had an experience of a loved one having a brain tumour (seriously, they’re more common than you might think).
I was hoping I didn’t get an appointment letter or phone call anytime soon as that would mean I needed surgery during the pandemic, which I really didn’t want to happen. But, I did get the referral letter, and I was booked in for a video consultation. I was petrified.
“Why do you think I needed to see you face to face,” said the surgeon, and, I said, “because you’re going to tell me it’s in a weird place and we can’t watch and wait, it has to come out”.
Brain Surgery
I am glad I had a surgeon who totally believed my symptoms were down to the tumour and it wasn’t really an “incidental finding” at all. Some people battle for years to get that across. I’ve had migraines for 25 years, and until I saw my neurosurgeon, everyone kept saying it was probably an atypical migraine.
I was booked in to have brain surgery for the 7th September. The day of my surgery, I felt great and was positive. I went into the theatre at 11am and came back to the ward at 7:30pm after telling my family and friends I’d be gone for about 4 hours. It must have been terribly worrying for them.
My surgeon said that when she got in there, it was in a really tricky place, so I ended up with 3 consultant neurosurgeons doing my operation. They still managed to remove all the tumour which was great.
The day after my surgery was awful. I wasn’t even able to check in with my family and friends to have some moral support and also give them some comfort as they were all anxious about me. I felt very sick and threw up all over the CT room, where I went for a post-op scan.
I desperately wanted to get home, and from the madness that was going on around the hospital, I pushed to be discharged on the Friday 11th. In hindsight, I shouldn’t have been so pushy to get home and should’ve accepted when my surgeons said I’d be in for ‘about a week’.
Post-Op
The first week or so, I had the most awful ‘squelching’ sensation every time I moved my head. I mentioned this in the hospital, and they showed me my scan, which showed pockets of air between my brain and skull. It felt like it wouldn’t go away, but that has mostly resolved now.
I’m taking regular pain relief (paracetamol and ibuprofen as well as codeine), anti-sickness medication, and laxatives (because both the anti-sickness and the codeine really horribly bung you up!) but genuinely I feel better than I imagined I would be feeling at this stage.
The thing everyone warned me about was the tiredness, and it really is as overwhelming as everyone says! I imagine I’ll be pretty tired for a good while yet. Still, I’m not doing much – making sure I get up and dress each day and eat what I fancy (my appetite has definitely been affected), I see the positive in the lockdown in that it’s not like I could go anywhere even if I felt up to it.
I can’t drive, for 6 months! which is a massive inconvenience. I have notified the DVLA and surrendered my licence and marked my car as being off the road. It’s only for a short time, so I can focus on the fact I won’t be reliant on public transport forever.
I think my life changed more from diagnosis to surgery. I had a constant headache for 4 months, and dizziness, and nausea. This, coupled with trying to be hypervigilant of any ‘red flag’ signs of hydrocephalus meant I spent that time very much worrying about ‘what if.’
I’m pretty confident that my life will get back to normal in time.
I’m fortunate that my surgeons are confident they got it all, so any chance of regrowth is negligible. Lots of people report memory and cognitive impairment post colloid cyst removal surgery. However, I don’t think I’ve got any, and my family and friends have all reported that I still seem very much myself.
My biggest fear of pre-surgery was being cognitively impaired. I was terrified about this.
What was it like being in the hospital during the peak of Covid-19?
The hospital was bizarre. Far fewer people about A&E, in particular, was eerie. Being a nurse, I’ve never seen a hospital so “quiet” although there were still a lot of patients. I was on a “green” ward both times, so all patients were negative for Covid-19, but staff even wore full PPE.
Were you happy having video consultations or would you have preferred meeting the doctor face to face?
I was happy with video consultations. Going for the face to face appointments, I had scans, pre-op, and appointments where I was consented for surgery were horrible, so many people seemed to struggle with maintaining social distancing.
I could see other people at my appointments had someone else with them. I felt very alone being me, myself and I.
Did your father have similar symptoms to his diagnosis?
My Dad’s symptoms were that he started feeling some weakness in his left leg and went to the GP as he thought he had sciatica.
The GP agreed this was probably the right diagnosis and prescribed anti-inflammatory medication and referred him for a scan.
His symptoms got progressively worse, and the GP suggested physiotherapy. The physiotherapist recognised that as his weakness was now affecting his whole left side, it probably wasn’t sciatica after all and arranged for him to be admitted to hospital for a scan as an inpatient.
His first scan was a lumbar spine scan on Friday and didn’t show anything out of the ordinary, so they decided to do a full spine scan on the Monday – over the weekend he fell and admitted that he had no sensation at all on his left side from his face to his toes.
The hospital decided to scan his head at the same time to rule out a stroke mostly, and it was then that his Glioblastoma Multiforme was found.
My Dad always said he felt fine after his surgery. Because of the type of tumour he had, he had to start aggressive daily radio and chemotherapy 2 weeks post-op which he said were much worse than the surgery.

How has your father shaped you in some way?
My Dad – he so very bravely fought for 10 months from his diagnosis to the day he died. We always knew his diagnosis was terminal, and he never once moaned or was negative. He will always be my hero.
I wasn’t a nurse when my Dad was diagnosed. I wasn’t a nurse when my Dad died. But nearly 3 years after he died of his brain tumour I resolved to be the best nurse I could be and to make a positive difference to as many people as I could and went back to university at 25.
I didn’t expect that 10 years later I too would have a brain tumour – because nobody expects that, but when I’ve recovered, I am absolutely going to make sure that I use my experience and my fathers to continue to try and help as many people as possible.
“I am absolutely going to make sure that I use my experience and my fathers to continue to try and help as many people as possible.”
Have you found any support post-surgery?
There are 2 specific colloid cyst support groups on Facebook that I joined. I’ve got mixed feelings about how helpful I’ve found them as I think there’s definitely some truth in what someone told me:
“The people who have great experiences are too busy getting on with life because they’re fully recovered, so they don’t stick around for years, the people who are still contributing actively are very often the people who had the worst outcomes. They’re still looking for support and a community to be a part of”
I think this is quite accurate, some of the members are amazing and positive and have made full recoveries and are getting on with their lives, but others have been left with really horrible symptoms from their tumours and the treatments they’ve had.
When I was first diagnosed, I spent a lot of time reading medical research on colloid cysts and patient outcomes. I was mainly able to do this because I have access, as a nurse, to years of medical journals. A lot of published research is quite scary. It talks about there being a 10-20% chance of sudden death, and 30-40% chance of sudden deterioration with colloid cysts and those are some alarming numbers! I talked them through with my neurosurgeon, and she was really reassuring.
I found reading Claire Snyman’s Book – Two Steps Forward really helpful. She is incredibly positive and writes brilliantly.
There was a lady on the ward who had also had a non-cancerous tumour removed who was also really positive, so it was nice to be able to chat with her.
Because of lockdown, I haven’t really heard of any ‘in real life’ support groups – but I have the most amazing family and a group of friends who have been the best support group I could’ve asked for. I do think sometimes it’s beneficial to talk things through with people who have similar experiences and who are less emotionally attached than your friends and family are, I look forward to meeting others at some point.
Any advice for people or loved ones that get daunting diagnoses?
- I think the best advice I could give is to ask questions – ask away, but take the answers in context depending on who is answering.
- Your family will want to protect you, people with personal experience will be more likely to apply what happened to them as fact, google is a scary place – especially on page 5 of results, at 3am when you can’t sleep.
- Your neurosurgeon, their team, and health professionals are the best people to ask. They will give you honest, objective answers.
- Use your experiences to shape your life in a positive way. I can’t tell you that everything will be OK, I can’t say that everyone will be fully cured and go back to life as normal. But I can tell you that you can use your experiences in a positive way.
- There isn’t a silver cloud to a brain tumour, but our experiences shape us, and we can choose to either focus on the new normal in a positive way, or dwell on what life was like before.
What motivates you?
I have an amazing family – my Nephew and Niece are absolutely my favourite people in the whole wide world. My tumour was found on my nieces 2nd birthday, so I’m going to have to spend at least the next 20 years making up for ruining her socially distanced garden visit party!
I absolutely adore my friends – even though they formed a support group called Friends Around Removed Tumours and very much sided with the tumour over me. My friends have held my hand through losing a parent at 22 to a brain tumour, and then getting one of my own at 35. I couldn’t ask for better friends.
I have the best job on earth. Digital Transformation Lead for The National Care Forum – the membership body for not for profit social care providers in England. I get to do exactly what I set out to do when I said I wanted to be a nurse. I get to support so many people to provide the people they care for with the best experiences by supporting them to embrace technology. My colleagues are amazing people.
Last year I was fortunate enough to be invited out to Australia to keynote at HIMSS Australia Digital Health Summit, and I’m motivated by the prospect of getting back to being that person!
Tell us something about yourself that people probably didn’t know… anything?
If you’ve read this far you probably know anything even vaguely interesting about me – I’m a pretty open book, to be honest, and always happy to overshare. One thing people might not know is that I contributed to a textbook when I was at university. And it’s nothing to do with nursing at all! It’s called “enhancing learning through technology.”
Find Claire Here:
TWITTER: @clairelsutton
INSTAGRAM: @clurrr_camera





Great to read that you are getting stronger and are still so positive