
Jane’s thalamic glioma story began when she visited her GP with memory symptoms she thought might be linked to perimenopause. Instead, that appointment marked the start of a brain tumour journey that led to a life-changing diagnosis and a watch-and-wait treatment plan.
When Jane went to see her GP at the start of the year, she thought she was dealing with symptoms of perimenopause.
Like many women, she had been encouraged by the growing conversation around menopause and hormone health, and wanted to explore whether HRT might help. A brain tumour was the very last thing on her mind.
But during the appointment, her GP became concerned about Jane’s memory symptoms and referred her for a CT scan.
At the time, Jane was not especially worried.
Three weeks passed without any news, and she assumed that was a good sign. Then, on 21 March, everything changed.
At 7.30 in the morning, she received a text asking her to come urgently to the GP surgery to discuss her scan results.
“I remember thinking, that doesn’t sound good,” Jane says.
She took her husband, Simon, with her. At first, she planned for him to stay in the waiting room, but at the last minute, she asked him to come in with her.
In the consultation room, Jane was told that abnormalities had been found in her brain. Doctors initially believed there were two tumours and that it could be a multifocal glioma. She was told she would need an MRI scan and that brain surgery, radiotherapy and chemotherapy might all be ahead of her.
“How is this happening? I didn’t feel that unwell.”
“It was devastating,” she says. “We walked out of the surgery in a complete blur.”
Outside the GP practice, Jane and Simon stood holding each other tightly as they both sobbed.
“I didn’t care who saw,” she says. “I just kept thinking, how is this happening? I didn’t feel that unwell. I couldn’t believe what I was hearing.”
Watch Jane tell her story in full in the Aunty M Brain Tumours Talk Show interview below, or keep reading for the written version
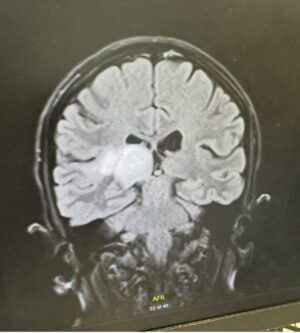
A few weeks later, Jane met with a surgeon and finally received some better news: there was only one tumour, not two.
That meant it was no longer thought to be a multifocal glioma. But there was still huge uncertainty. The tumour was in Jane’s thalamus, a deep and highly sensitive part of the brain that acts as a central relay point for signals travelling in and out.
Because of the location, surgery to remove it was ruled out.
“I knew in that moment that my odds had reduced quite significantly,” Jane says. “That was frightening.”
A biopsy was offered as a possible next step, but it came with serious risks. Jane describes the consultation as overwhelming, with the dangers of surgery explained in such stark detail that she and Simon were left frozen with fear.
At first, it felt as though there was no real choice. She would simply have to be brave and go through treatment.
But after speaking to an oncologist, talking with family and friends, and doing her own research, Jane began to feel that active surveillance might be the right option for now.

Today, Jane is being monitored with MRI scans every three months.
Doctors believe the tumour is likely to be low-grade. It is not currently showing signs of swelling or aggressive behaviour, which is reassuring. But because Jane has not had a biopsy, there is still no definitive diagnosis.
That uncertainty is one of the hardest parts.
“I don’t know exactly what tumour type I have,” she says. “I’ve heard a couple of different opinions, so I’m not quite sure what lane I’m in.”
For now, active surveillance means no treatment unless the tumour changes, symptoms appear, or Jane decides she wants to pursue a biopsy.
But living in a “watch and wait” situation brings its own emotional strain.
Because she has not had seizures and is not experiencing symptoms directly linked to the tumour, Jane often feels caught between being told she has a brain tumour and yet not actively “doing” anything about it.
That can make every small ache, twinge or headache feel loaded with meaning.
“Every little thing makes you think, it’s coming, it’s coming. You have to work really hard not to let those thoughts take over.” she says.
The scans themselves bring both stress and relief. In some ways, Jane says she almost looks forward to them, because a clear result gives her precious reassurance for a while. But as the next scan approaches, the fear begins to creep back in.
Finding support that truly understands
Jane says support from brain tumour charities has made an enormous difference to her and her family.
She reached out to a brain tumour charity advice line in one of her darkest moments and found comfort in speaking to someone who truly understood.
“Sometimes it’s not even about being emotional,” she says. “It’s just about talking to someone who gets it. You have to understand how awful having a brain tumour is, and only people who either have it or work in that field really do.”
She has also had formal counselling, which she describes as incredibly helpful.
That support extended beyond Jane herself. With a 10-year-old daughter at home, Jane and Simon faced the heartbreaking task of explaining the diagnosis in a way their child could understand. Specialist support helped guide those conversations and gave them confidence in how to handle such a difficult situation.
Further counselling and play therapy for their daughter has also been invaluable.
Jane is clear that, without the help of these charities, her family would not have got through the past year in the same way.
“They’ve been amazing,” she says. “They’ve helped our family so much.”
Turning pain into purpose
Rather than let the anniversary of her diagnosis be defined only by fear, Jane has chosen to turn it into something joyful.
On 21 March 2026, one year on from the day her world changed, she will be holding a charity concert at St Andrew’s Church in Backwell, North Somerset.
The event will celebrate Jane’s love of 90s and noughties dance music, reimagined with an orchestral twist.
Think club classics, disco lights, a red carpet, a big disco ball, drinks, dressing up, and a village church transformed for one unforgettable night.
“It’s a bit unusual for a church,” Jane laughs. “But somehow I managed to persuade the vicar.”
Planning the concert has become more than fundraising. It has been a lifeline.
“It’s given me a really good distraction from everything I’ve been going through,” she says. “This is another form of therapy for me.”
Jane has already received incredible community support, from raffle prizes to practical help, and says the whole process has brought her real joy and purpose.
She has also found strength in speaking openly online, using Instagram and video diaries to document her experience and connect with others.
“This isn’t who I thought I was,” she says. “But it’s who I need to be right now.”
Love in the trenches
When Jane reflects on who has carried her through this experience, her answer is immediate: her husband, Simon.
“I don’t know how he’s got through it, if I’m honest,” she says. “If it was the other way round, I think I’d be a complete wreck.”
She describes clinging to him, crying into him, and leaning on him in ways she never had before. Through it all, he has stayed by her side, gone to every appointment, absorbed every fear, and stood in the trenches with her.
“It feels like we both have the tumour,” she says.
And amid all the shock, grief and uncertainty, Jane says there has also been one unexpected silver lining: a deeper understanding of just how loved she is.
“I’ve realised how much he loves me,” she says. “And that’s pretty special.”
Follow Jane on Instagram @memybraintumourandi. Where she shares her video diaries.
Jane’s story is a reminder that brain tumours do not always present in obvious ways. Symptoms can sometimes be vague and may be mistaken for other health issues.
It is also a reminder that:
- every brain tumour journey is different
- not all tumours can be operated on
- “watch and wait” can be an active and appropriate treatment plan
- emotional support matters just as much as medical care
- specialist charities can make a life-changing difference for patients and families
Behind every diagnosis is a person, a family, and a life that changes in an instant.
Jane’s story shows the reality of living with uncertainty, but also the power of support, honesty, community and finding purpose even in the most difficult circumstances.
Follow Jane on Instagram @memybraintumourandi. Where she shares her video diaries.
Here are the Places Jane mentioned:
The BrainTumour Charity
The Brain Tumour Support
Brainstrust
View this post on Instagram
Understanding Thalamic Glioma:
Jane’s tumour is believed to be a thalamic glioma. That means it is a glioma located in the thalamus, a deep part of the brain.
What is the thalamus?
The thalamus is a small but very important structure near the centre of the brain. It acts a bit like a relay station, helping to pass information between different parts of the brain and body. It plays a role in things like:
- movement
- sensation
- alertness
- sleep
- memory and thinking
Because the thalamus sits so deep in the brain and is involved in many vital functions, tumours in this area can be especially difficult to treat with surgery.
What is a glioma?
A glioma is a type of brain tumour that starts in the brain’s glial cells. These are the cells that support and protect nerve cells.
Gliomas can behave very differently from one person to another. Some are low grade, meaning they tend to grow more slowly. Others are high grade, meaning they are more aggressive and faster growing.
In Jane’s case, doctors believe the tumour is likely to be low grade, which is reassuring, but because she has not had a biopsy, there is still some uncertainty about the exact tumour type.
Why might surgery not be possible?
One of the biggest challenges with a thalamic glioma is its location.
Even when a tumour is small or appears slow growing, operating in the thalamus can carry a significant risk because this part of the brain is surrounded by structures that control essential functions. For some patients, surgery to remove the tumour is not possible, and doctors may instead consider:
- biopsy
- radiotherapy
- chemotherapy
- active surveillance with regular scans
The right option depends on the tumour’s size, position, behaviour, symptoms, and the risks of treatment.
What does “active surveillance” mean?
Active surveillance — sometimes called watch and wait — means doctors monitor the tumour closely with regular MRI scans instead of starting treatment straight away.
This approach may be recommended when:
- The tumour appears low-grade
- it is not currently causing significant symptoms
- treatment risks may outweigh the benefits at that stage
- doctors want to monitor whether the tumour changes over time
Active surveillance does not mean nothing is happening. It means the medical team is carefully watching for any sign that the tumour is growing or changing.
Why uncertainty can be so difficult
One of the hardest parts of a brain tumour diagnosis can be the not knowing.
Some people have a clear diagnosis after surgery or biopsy. Others, like Jane, may live with uncertainty about the exact tumour type while scans continue. That uncertainty can have a huge emotional impact, especially when someone is feeling physically quite well but living with the knowledge that a brain tumour is there.
DISCLAIMER: This information is for general awareness only and is not a substitute for advice from your own medical team. Aunty M Brain Tumours shares personal experiences and supportive information, not individual medical guidance.
View this post on Instagram



